Utilization of a 3D bioprinted liver tissue model to evaluate the antifibrotic effects of an ALK5 inhibitor in a TGFβ-induced model of hepatic fibrosis
Publication Summary:
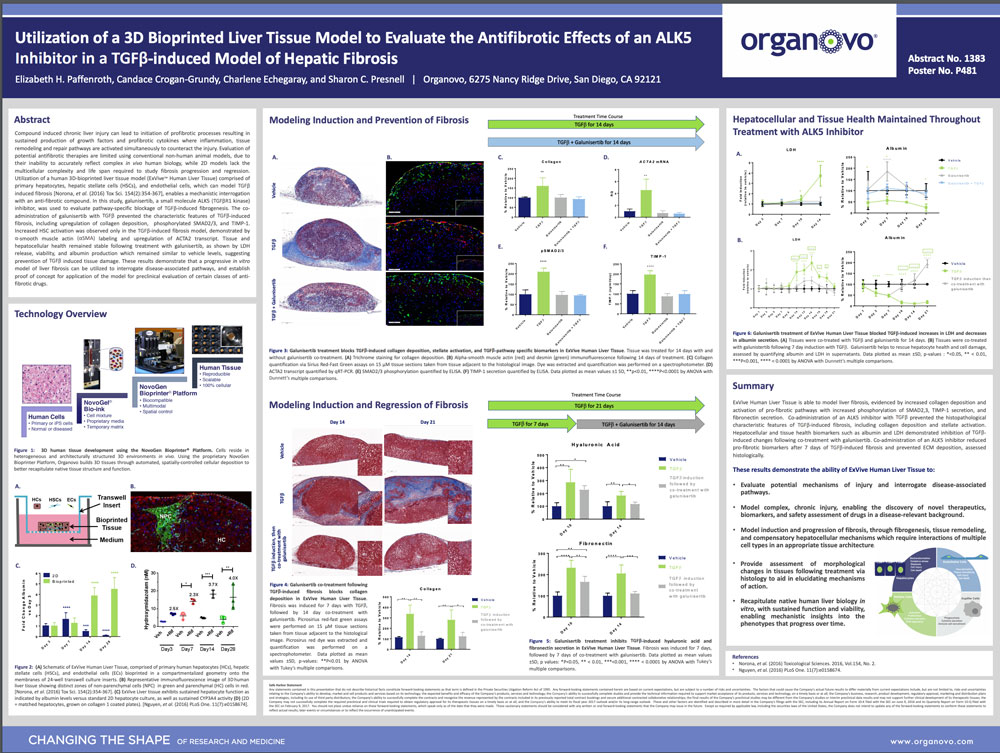
Compound induced chronic liver injury can lead to initiation of profibrotic processes resulting in sustained production of growth factors and profibrotic cytokines where inflammation, tissue remodeling and repair pathways are activated simultaneously to counteract the injury. Evaluation of potential antifibrotic therapies are limited using conventional non-human animal models, due to their inability to accurately reflect complex in vivo human biology, while 2D models lack the multicellular complexity and life span required to study fibrosis progression and regression. Utilization of a human 3D-bioprinted liver tissue model (ExVive™ Human Liver Tissue) comprised of primary hepatocytes, hepatic stellate cells (HSCs), and endothelial cells, which can model TGFβ induced fibrosis [Norona, et al. (2016) Tox Sci. 154(2):354-367], enables a mechanistic interrogation with an anti-fibrotic compound. In this study, galunisertib, a small molecule ALK5 (TGFβR1 kinase) inhibitor, was used to evaluate pathway-specific blockage of TGFβ-induced fibrogenesis. The coadministration of galunisertib with TGFβ prevented the characteristic features of TGFβ-induced fibrosis, including upregulation of collagen deposition, phosphorylated SMAD2/3, and TIMP-1. Increased HSC activation was observed only in the TGFβ-induced fibrosis model, demonstrated by α-smooth muscle actin (αSMA) labeling and upregulation of ACTA2 transcript. Tissue and hepatocellular health remained stable following treatment with galunisertib, as shown by LDH release, viability, and albumin production which remained similar to vehicle levels, suggesting prevention of TGFβ induced tissue damage. These results demonstrate that a progressive in vitro model of liver fibrosis can be utilized to interrogate disease-associated pathways, and establish proof of concept for application of the model for preclinical evaluation of certain classes of antifibrotic drugs.
View Publication